|
Runners commonly have issues with piriformis syndrome, which is a literal pain in the butt, but it is difficult to determine the cause, so we are going to take a peek at functional anatomy and what research has supported in the treatment of piriformis syndrome.
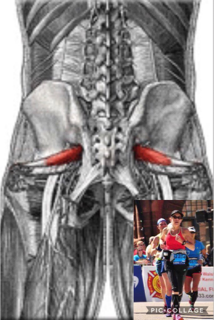
As a very basic description, the piriformis muscle arises from the front portion of the sacrum (tailbone) and attaches to the femur (thigh bone) and its main function is hip external rotation (thigh bone rotating in an outward direction), aids in hip abduction (thigh away from the body), and aids in hip extension. Hip extension is what creates forward propulsion of the body during running. Due to my experiences with runners, I always think of the orientation and relationship of the pirifomis with the gluteal muscles. Dr. Shirley Sahrmann (2002) discusses the synergistic relationship of the piriformis with the gluteus maximus (GM) in hip extension. The GM is the main muscle of hip extension and the piriformis is one of the “helpers” in hip extension. Like all muscles, the piriformis may be subject to pain associated with muscle shortening from overuse as seen in synergistic dominance. Synergistic dominance is what occurs when a prime mover muscle is shut down and the helper muscle picks up all the work, making it too big for your britches, or just too tight and strong. Dr. Sahrmann does mention that the GM is a muscle that is frequently weak and the piriformis work load increases. Pain may also be from weakness of the muscle from lengthening. This pain is a literal pain in the butt and I unfortunately have had an issue with a weak, lengthened piriformis muscle, as diagnosed by a physical therapist (PT) a few years ago. I specifically remember the PT telling me, “Your marathon training is asking your gluteal muscles and pirifromis to do something they’re not strong enough to do.” I was reminded of this when Dr, Sahrmann said that it is a misconception that participating in a sport places adequate demands on musculature to elicit normal performance. In my case, I thought the dynamic nature of running would be enough strengthening of my running muscles to avoid weaknesses. This is a strong case for prehab exercises. I am all for prevention instead intervention, which is the point of many of my blog posts! Tonley and colleagues discuss piriformis syndrome in a 2010 case report of a subject complaining of “deep buttock pain”. The authors theorized that when the GM is weak, it accommodates abnormal movement patterns at the hip and consequently contributing to excessive lengthening of the pirifomis during functional activities. Muscle testing revealed weakness in the hip abductors, extensors, and external rotators. The subject participated in eight physical therapy sessions during a 3-month intervention. The intervention included exercises that were done at home in three, 4-week progressive exercises phases. Two weeks post intervention the subject declared no buttock pain and increased strength in the hip abductors, extensors, and external rotators. One year post intervention the subject still reported remaining pain free in the buttocks and had resumed sporting activities that were sidelined by pain. I think it is important to point out that synergistic dominance and muscle lengthening is often due to what we are doing when we aren’t running; sitting in the car, sitting at your work space, sitting on the couch, sitting in the bar, sitting with your legs crossed…sitting! Don’t ever forget movement is medicine and the one hour you may spend running, has nothing on all the hours of sitting throughout the day! By the way, if you want to know what the exercises in the pirifomis syndrome case study were, contact me at runwithgina@gmail.com Fight ON! Coach Gina Runner Image: Kay Kay Weir References: Sahrmann, S. A., (2002). Diagnosis and treatment of movement impairment syndromes. Philadelphia, PA: Mosby. Tonley, J. C., Yun, S. M., Kochevar, R. J., Dye, J. A., Farrokhi, S., & Powers, C. M. (2010). Treatment of an individual with piriformis syndrome focusing on hip muscle strengthening and movement reeducation: A case report. Journal of Orthopaedic & Sports Physical Therapy, 40(2), 103-111.
0 Comments
Leave a Reply. |
Archives
October 2021
Categories |
 RSS Feed
RSS Feed